Who Needs Laparoscopic Hysterectomy? Conditions & Symptoms Explained
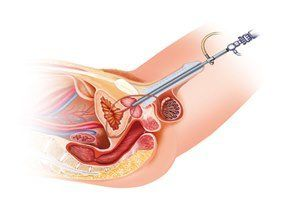
When gynecological problems start affecting daily life, long-term health, and emotional well-being, surgery may become a necessary option. One of the most advanced and patient-friendly surgical solutions today is laparoscopic hysterectomy. If you are experiencing persistent gynecological symptoms, consulting an experienced Laparoscopic Hysterectomy surgeon in Aundh can help you understand whether this minimally invasive procedure is right for you. What Is Laparoscopic Hysterectomy? Laparoscopic hysterectomy is a minimally invasive surgical procedure used to remove the uterus through small incisions in the abdomen. A tiny camera (laparoscope) and specialized instruments allow the surgeon to perform the surgery with precision, minimal pain, and faster recovery compared to traditional open surgery. Depending on the medical condition, the procedure may involve removal of: Only the uterus Uterus and cervix Uterus along with ovaries and fallopian tubes This approach is widely preferred today due to its safety and effectiveness. Who May Need Laparoscopic Hysterectomy? Laparoscopic hysterectomy is usually recommended for women who suffer from chronic gynecological conditions that do not improve with medications or conservative treatments. It is especially considered when symptoms significantly interfere with quality of life. Women With Long-Standing Gynecological Problems If pelvic pain, abnormal bleeding, or pressure symptoms persist despite treatment, hysterectomy may offer permanent relief. Women Who Have Completed Their Family Since hysterectomy ends the possibility of pregnancy, it is typically advised for women who do not plan future pregnancies after careful consultation with their doctor. Common Medical Conditions That Require Laparoscopic Hysterectomy Uterine Fibroids Fibroids are non-cancerous growths in the uterus that can cause heavy bleeding, pelvic pain, bloating, and pressure on the bladder. When fibroids are large, multiple, or cause severe symptoms, laparoscopic hysterectomy is often the most effective solution. Adenomyosis Adenomyosis occurs when the inner lining of the uterus grows into the uterine muscle, leading to painful periods and excessive bleeding. In severe cases, hysterectomy provides lasting relief when medications fail. Endometriosis (Severe Cases) Endometriosis can cause chronic pelvic pain and painful intercourse. When the condition is advanced and unresponsive to treatment, hysterectomy may be recommended to improve quality of life. Abnormal Uterine Bleeding Uncontrolled or prolonged menstrual bleeding can lead to anemia, fatigue, and weakness. When hormonal therapy and minor procedures do not work, hysterectomy becomes a definitive treatment. Uterine Prolapse Uterine prolapse occurs when the uterus descends into the vaginal canal due to weakened pelvic muscles. Laparoscopic hysterectomy offers a less invasive and effective surgical solution for moderate to severe prolapse. Early-Stage Gynecological Cancer In certain early-stage cancers of the uterus or cervix, hysterectomy plays a crucial role in treatment and prevention of disease progression. Symptoms That Indicate You May Need a Hysterectomy Women experiencing the following symptoms should seek medical evaluation: Heavy or prolonged menstrual bleeding Severe pelvic or lower back pain Pain during sexual intercourse Pressure on the bladder or bowel Frequent urination Chronic anemia and fatigue No improvement with medications or hormonal therapy Early diagnosis can help determine whether hysterectomy is necessary or if other treatments are possible. Why Doctors Recommend Laparoscopic Hysterectomy Laparoscopic hysterectomy has become the preferred choice due to several benefits: Smaller incisions and minimal scarring Less pain and reduced blood loss Faster recovery and early return to normal activities Shorter hospital stay Lower risk of infection and complications This advanced technique ensures better outcomes and patient comfort. Who Is Not an Ideal Candidate for Laparoscopic Hysterectomy? Although laparoscopic hysterectomy is safe for most women, it may not be suitable in certain cases such as: Extremely large uterus (decision depends on surgeon expertise) Severe uncontrolled medical conditions Advanced gynecological cancer requiring open surgery A thorough medical evaluation is necessary before making a surgical decision. How Is the Decision for Hysterectomy Made? The decision to undergo hysterectomy is based on: Detailed medical history Physical and pelvic examination Ultrasound or MRI reports Severity of symptoms Patient’s age and overall health An experienced Gynecologist in Aundh will discuss all available treatment options and guide you toward the best possible decision. When Should You Consult a Gynecologist? You should consult a gynecologist if: Symptoms persist for more than 3–6 months Menstrual bleeding becomes heavy or irregular Pelvic pain affects daily activities Medical treatment does not provide relief Early consultation helps prevent complications and improves long-term health outcomes. Conclusion Laparoscopic hysterectomy is a highly effective solution for women suffering from chronic gynecological conditions that do not respond to other treatments. Early diagnosis, proper evaluation, and expert guidance are essential for achieving the best results. If you are experiencing persistent symptoms, consulting an experienced Laparoscopic Hysterectomy surgeon in Aundh can help you regain comfort, confidence, and a better quality of life. FAQs Is laparoscopic hysterectomy safe? Yes, it is a safe and widely performed procedure when done by an experienced surgeon. Will periods stop after hysterectomy? Yes, periods stop permanently after removal of the uterus. How long does recovery take? Most women resume normal activities within 2–4 weeks. Are ovaries removed during hysterectomy? Ovaries may be preserved depending on age and medical condition.